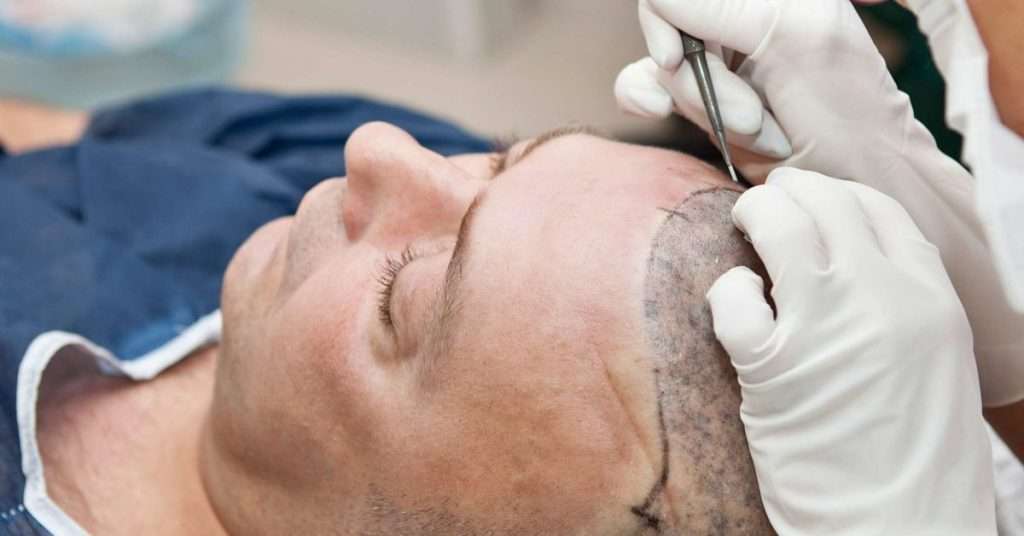
“The work we are doing today is the logical next step in improving the outcomes of hair transplant surgery procedures. These double-blind, controlled studies approved by the Western Institutional Review Board are necessary to properly evaluate the use of a nonhuman extracellular matrix (ECM) for improving hair transplant procedure outcomes,” says Dr. Robert M. Bernstein, hair transplant surgeon and founder of Bernstein Medical — Center for Hair Restoration in New York City, who is leading the study.
What is a nonhuman extracellular matrix?
ECM, the substance found between all animal cells and made up of fibrous proteins, provides support for cells, regulates intercellular communication and provides growth factors for wound healing and tissue regeneration. “We are specifically using ACell MatriStem extracellular matrix, which is biologically derived from a pig and has been found to be nonantigenic, meaning it is not susceptible to rejection by humans. We are investigating the many ways this nonhuman ECM can be used to improve hair transplant procedures,” explains Bernstein.
Implications for scar improvement in hair transplant surgery
A challenge in hair transplant surgery has been to minimize scarring where the donor hair has been taken. “Previously,” Bernstein explains, “if someone has a donor scar, trying to cut out the scar may create more scarring. We have been testing the use of ECM by placing it into the donor incision in order to facilitate healing and make the scar finer. What we found, instead, is that it makes the scar suppler and more amenable to putting in new hair as the scar heals, enabling us to camouflage the scar rather than risk trying to remove it.”
Implications for multiplying hairs to increase a person’s hair donor supply for hair transplants
In the p ast a person was limited in a hair transplant by how much donor hair he or she had to spare. “If we can multiply the hairs a person has, then we have more hair to work with, so this research has broad implications for hair transplant procedures,” explains Bernstein. “Hair cloning is really just multiplying hairs. We try to stimulate a whole follicle to grow from a partial follicle, either derived from plucked hair or by sectioning the follicle. “Past hair cloning procedures were performed by attempting to multiply hair-producing cells outside of the body. And it was found that if researchers tried to multiply the cells outside the body, they quickly stopped making hair. Even when these in vitro cells were injected into the scalp, cosmetically useful hair wouldn’t develop. “In these new studies we are using ECM to prime the holes that the plucked hairs, or sectioned follicles, are being placed into to see if they can be induced to grow. Our preliminary studies are showing that this works to some degree. Other variables, such as using platelet-rich plasma (PRP) for its wound-healing and growth-stimulating properties, are being tested as well. Researchers are trying many different variations to see if we can get these plucked hairs and sectioned follicles to grow.”
Bernstein continues, “If we can get these cells to grow, the next question is where the genes in this new hair follicle are coming from. Are they coming from the plucked hair or the surrounding skin to form a full follicle?” Hair transplant success has always been based on the scientific theory of “donor dominance,” which means the transplanted cells retain the characteristics of where they came from — in this case, resistant to the androgens (hormones) that cause male pattern baldness. “If we can multiply these androgen-resistant hairs, we don’t use up the limited amount of donor hair. We don’t know, yet, the full practical uses of what we are studying, and that’s what’s so exciting,” he concludes.
The rest of the hair transplant community shares Bernstein’s anticipation. “The possibility of having an unlimited supply of donor hair on hand to treat hair loss is exciting,” adds Dr. David S. Orentreich, New York City hair loss treatment specialist, board-certified dermatologist and partner of the Orentreich Medical Group. “We encourage and look forward to further tissue engineering-based research that Dr. Bernstein and others are doing to triumph over the obstacles we presently face in the field of hair restoration surgery.”